Hypothyroidism and diabetes tend to go hand-in-hand.
In fact, here’s something most people have never been told…
When your body struggles to regulate blood sugar effectively, it can make it more difficult for your cells to use thyroid hormone efficiently.
And when thyroid function is low, your body may also have a harder time maintaining stable blood sugar levels.
In other words…
These two issues are deeply connected — far more than most people realize.

In fact, many people struggling with thyroid and blood sugar imbalances don’t realize how closely these systems influence each other.
And in this article, based largely on the work of Dr. Raymond Peat, we’re going to show you how this connection works — and what you can do to support better energy and blood sugar balance.
But first…
You need to understand something that most people — and even some conventional approaches — tend to overlook.
Why Thyroid and Blood Sugar Issues Are Not About Sugar
Today, diabetes is often blamed directly on sugar.
You’ve probably heard it called the “sugar disease.”
And on the surface, that might seem to make sense…
You eat sugar → your blood sugar rises → and over time, that can create problems.
But let me ask you something…
Imagine you have a clogged sink drain while the water is running.
As the water level rises higher and higher… do you blame the water?
Of course not.
You fix the clog.
So why are we treating blood sugar any differently?
Here’s the problem…
Focusing only on sugar misses what’s actually going on beneath the surface.
Because diabetes isn’t just about how much sugar is in your blood…
It’s about how well your body is able to use that sugar.
This is where the relationship between thyroid and blood sugar becomes especially important.
The Real Issue — How Thyroid Function Affects Blood Sugar at the Cellular Level
Your body relies on glucose as one of its primary fuel sources.
But in order for that fuel to be useful, it has to get inside your cells.
That process depends on insulin…
And more importantly — how responsive your cells are to insulin.
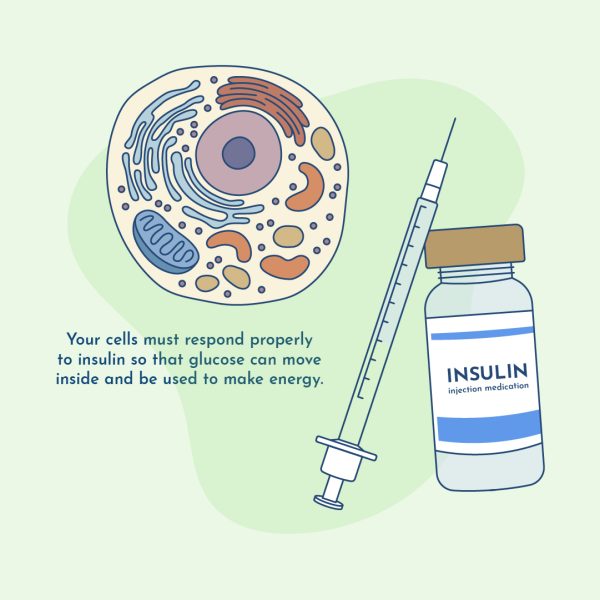
When that system isn’t working properly, glucose can build up in your bloodstream… even if you’re barely eating carbohydrates.
In other words…
Lowering sugar intake doesn’t actually fix the problem.
Because the real issue is how your body is handling energy at the cellular level.
And when it comes to thyroid and blood sugar, this cellular energy process is where most problems begin.
How Thyroid and Blood Sugar Become Linked
Now let’s zoom out and look at the bigger picture…
Because this is where things start to click.
The Randle Cycle — When Fat Blocks Sugar
There’s a well-documented mechanism called the Randle Cycle.
In simple terms…
When higher levels of fats are circulating in your bloodstream, they can compete with glucose and make it harder for your cells to use it efficiently.
So instead of burning sugar for energy…
Your body shifts toward burning fat — and glucose starts to back up in the bloodstream.
This is one of the key patterns seen in insulin resistance.
This is also why insulin resistance and thyroid issues are often seen together.
What Happens to Blood Sugar When Thyroid Function Slows Down
Now here’s where it gets even more interesting…
When thyroid function slows down, several things begin to change.
Including how your body regulates blood sugar throughout the day.
1. Liver Glycogen Becomes Less Reliable
Your liver is supposed to store glucose in the form of glycogen…
And release it steadily between meals to keep your blood sugar stable.
But when this process isn’t working efficiently, your body has to compensate.
And that’s where stress hormones come in.
2. The Stress Hormone Cascade
When blood sugar starts to drop…
Your body releases adrenaline.
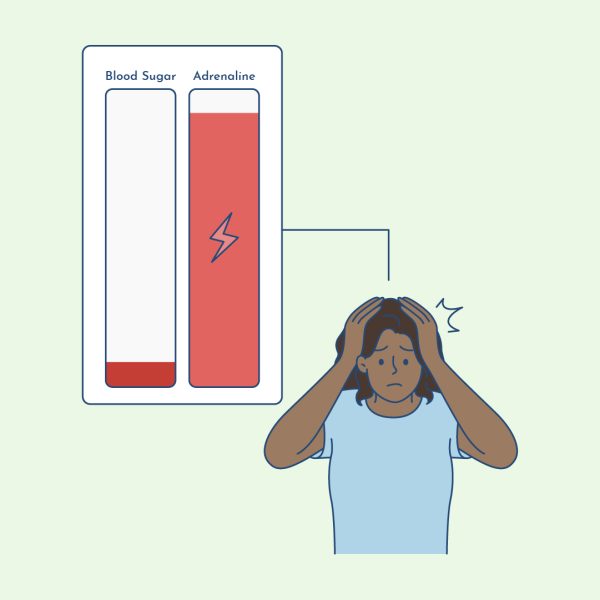
Why?
To keep you alive.
Adrenaline signals your body to release stored fuel — including fats — into the bloodstream.
And here’s where things start to spiral…
Adrenaline increases the release of stored fats into the bloodstream — which may interfere with how your cells use glucose and respond to insulin.
Over time, this can make it harder for your body to maintain stable blood sugar levels.
Then comes cortisol… another stress hormone that helps convert protein into glucose to keep your brain fueled.
Because your brain depends heavily on a steady supply of sugar to function.
So now you have this pattern:
- Stress hormones rise
- Blood sugar fluctuates
- Cells struggle to use fuel efficiently
And the cycle continues…
Which is why many people with thyroid issues also experience blood sugar swings, fatigue, and cravings.
3. The Role of Circulating Fats (PUFAs)
Now let’s take this one step further.
Because not all fats behave the same way.
When stress hormones release stored fats into your bloodstream…
Many of those fats come from polyunsaturated fats — or PUFAs — that have accumulated in your tissues over time.
And here’s where it matters:
Elevated levels of certain polyunsaturated fats (PUFAs) have been shown in some studies to negatively affect the function and overall health of insulin-producing beta cells.
And when these cells aren’t functioning optimally…
It can make it more difficult for your body to manage blood sugar effectively.
So now we have two major problems happening at the same time:
- Cells are less responsive to insulin
- And the cells that produce insulin may not be functioning optimally
That’s a tough cycle to break.
Especially when both thyroid and blood sugar regulation are being affected at the same time.
The Thyroid and Blood Sugar Vicious Cycle Explained
Put it all together, and here’s what happens:
- Blood sugar drops → stress hormones rise
- Stress hormones release fats → glucose use becomes less efficient
- Blood sugar rises → body compensates again
And over time…
This pattern reinforces itself.
Which is why simply focusing on avoiding sugar doesn’t solve the problem.
While minimizing PUFAs in your diet is important for supporting thyroid health, there are additional foods that can help provide even more support.
Some of those foods can be found in our 3 Food Thyroid-Boosting Daily Protocol.
You can download it for free here.
Why Low-Carb Diets Don’t Support Thyroid and Blood Sugar Balance
Now this might surprise you…
Because low-carb diets are often recommended for blood sugar control.
And yes — they can lower blood sugar in the short term.
But here’s the bigger picture:
When it comes to thyroid and blood sugar balance, the approach isn’t always as simple as cutting carbohydrates. For some people, long-term carbohydrate restriction may actually make it more difficult for the body to regulate blood sugar effectively.
Why?
Because when carbohydrates are consistently restricted…
Your body may rely more heavily on stress hormones to maintain stable energy.
And if those same stress hormones are part of what’s contributing to the problem…
You can see how this becomes counterproductive over time.
In other words…
Blood sugar may look better on paper…
…but the underlying issue hasn’t been addressed.
How to Actually Support Thyroid and Blood Sugar Balance
This is where most approaches fall short.
Because they focus on managing symptoms… instead of addressing the system underneath.
If the goal is long-term blood sugar stability, addressing the underlying factors that influence metabolic function is what makes the biggest difference.
So what does that look like?
It starts with supporting both thyroid function and blood sugar balance at the same time.
1. Support Stable Energy Through Diet
Instead of removing carbohydrates entirely…
The goal is to use them strategically.
Carbohydrates provide a key source of fuel your body depends on to maintain stable blood sugar and support efficient cellular energy production.

And when that fuel isn’t consistently available…
Your body is forced to compensate — often by increasing stress hormone output.
This is why balance matters.
Because thyroid and blood sugar stability both depend on a consistent and usable source of fuel.
2. Reduce Excess Circulating Fats
Another key piece is limiting the release of excess fats into the bloodstream…
Especially those that can interfere with glucose metabolism.
This helps support a more balanced fuel system.
3. Improve How Your Body Uses Energy
Ultimately, this comes back to your cells.
Because energy isn’t just about what you eat…
It’s about what your body can actually use.
And when your cells can use fuel efficiently again…
Everything starts to work better together.
A Simple Next Step
If you’re starting to see how this all connects… then the next step is simple.
We’ve put together a short, practical guide that walks you through how to begin supporting this process using just a few key foods.
It’s called the 3 Food Thyroid-Boosting Daily Protocol.
And you can download it for free here.
The Bottom Line
The truth is…
This isn’t about avoiding sugar.
And it’s not about extreme diets.
It’s about understanding how your body actually works.
Because once you do…
You stop chasing symptoms — and start supporting the system that drives everything.
And that’s when things finally start to change.

KEY IDEA
Most people are told blood sugar problems are caused by eating too much sugar… but that’s not the real the story. The real issue is how well your body can use that sugar — and this is where your thyroid plays a critical role. When thyroid function slows, your body relies more on stress hormones, releasing fats that can interfere with how your cells use glucose. Over time, this creates a cycle of unstable energy and blood sugar swings. That’s why simply cutting carbs doesn’t solve the problem, and can actually make things worse. The key is supporting how your body produces, stores, and uses energy — so blood sugar and energy can finally stabilize together.